People without an HMO or long-term health and disability insurance would have reason to worry. But if you have coverage, and have been making your premium payments on time every month, you have nothing to worry about, right?
Right???
The Great American Dream, indeed. For many, it is more like the great American nightmare.
At least it has been for Judy, who tells a woeful tale around trying to collect in vain from Unum after being injured on the job. A former acute care hemodialysis nurse from Portland, Judy had been working as part of an acute mobile unit that would visit several different hospitals.
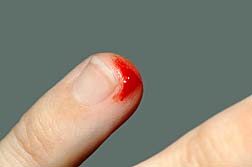 She writes that in 2004 she developed a serious, penicillin-resistant staph infection, which entered her bloodstream through a small paper cut on her finger. The infection proved extremely serious and confined her to hospital for several weeks. The infection left her with severe pain, and in critical condition for a prolonged period.
She writes that in 2004 she developed a serious, penicillin-resistant staph infection, which entered her bloodstream through a small paper cut on her finger. The infection proved extremely serious and confined her to hospital for several weeks. The infection left her with severe pain, and in critical condition for a prolonged period.Such are the hazards associated with being a nurse. Sometimes, in your work that is often described as selfless in the care and compassion of others, you get injured too.
That's what long term disability insurance is for. That's why you buy it, that's why you pay for it. It is an investment in your health and well-being, and that of your family and your dependants, in the event the unthinkable happens.
It would be unthinkable to be denied something for which you have already paid. Or so it seems. But don't tell that to an anonymous blogger with Ripoff Report, who claims to have toiled at one time as a claims associate with Unum Provident.
"We were always instructed to deny ALL claims as soon as they were received," the former claims associate wrote in 2006. "No matter what the disability and no matter what the situation was. ALL CLAIMS WERE DENIED (sic).
"Some people received these notices and never followed up. Others chose to pursue the matters. This meant that most of the time, initial denials did work to save the company money when claimants didn't respond.
"Fines paid by these companies for deceitful practices do not compare to the money they save by denying claims and destroying people's lives.
"I left the company after a very heated discussion of one of my claims. The claimant was an anesthesiologist who had suffered an injury to his hand and was unable to continue performing his occupation. The policy paid a substantial amount of money in monthly benefits if it were a normal person in any other occupation but it fell extremely short of covering his living expenses.
"Needless to say, at the instruction of my manager, I was forced to deny this claim over and over. This claimant lost his home, his vehicles, and other possessions but most importantly, he was forced to withdraw his children from college because he could no longer afford to pay."
Judy had a different problem. In her blog entry, the injured nurse relates that she was approved "not once, not twice but several times by Unum."
"But do they pay? No!"
She reports having waited 10 months for both short, and long-term disability payments, after her claim was apparently approved. Stalling tactics included repeated requests for information already sent and received (by registered mail, Judy reports).
READ MORE LEGAL NEWS
The new check never arrived. However, what did was a request for additional documentation, which added another month to the wait. Finally, a letter arrives congratulating Judy on the approval of her claim. This has already been approved, however. And the check, supposedly in the mail, never arrives.
Judy notes in her entry that she has had to sell her beautiful home and incur substantial debt, which has proven to be a strain on her new marriage. Thank goodness, she says, for her wonderful, understanding husband who has been so supportive throughout the mess.
"If I were single," she writes, "I would be homeless..."
