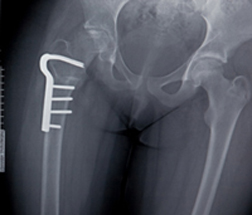
 The study concluded that there was no evidence seen of any increased risk for subtrochanteric or diaphyseal fractures to the femur bone in patients using bisphosphonates (Fosamax) as compared with those on a therapy of raloxifene/calcitonin.
The study concluded that there was no evidence seen of any increased risk for subtrochanteric or diaphyseal fractures to the femur bone in patients using bisphosphonates (Fosamax) as compared with those on a therapy of raloxifene/calcitonin."However, this study cannot exclude the possibility that long-term bisphosphonate use may increase the risk of these fractures."
In other words, while no evidence was found that Fosamax increased the risk of such fractures, the link between Fosamax and femur fractures was real enough to conclude that such a risk could exist over the long term.
Blogger Tom Lamb notes in a recent issue of Drug Injury Watch that a large cohort study originating in Sweden and published this month in the New England Journal of Medicine found that patients using bisphosphonates such as Fosamax to treat the effects of osteoporosis were 50 times more likely to suffer fractures to the femur shaft, when compared to control patients not using bisphosphonates.
Having said that, the study concluded that in spite of the foregoing, the absolute risk of suffering Fosamax femur fractures remained very low.
READ MORE FOSAMAX LEGAL NEWS
However, the study "ONJ in Two Dental Practice-Based Research Network Regions" concluded that the absolute risk for Fosamax osteonecrosis of the jaw was quite low.
Similar conclusions were reported at the 89th General Session and Exhibition of the International Association of Dental Research. According to Lamb and a March 2011 article in Medscape, oral bisphosphonates such as Fosamax were not seen to increase the risk for Fosamax dead jaw.
At the same time, however, intravenous bisphosphonates were shown to increase the risk for Fosamax osteonecrosis of the jaw by six times, over those patients who did not receive bisphosphonates through an IV. While there was no difference in the drug itself, the method of delivery appeared to play a factor.

READER COMMENTS
Harold Phillips
on