Los Angeles, CA: A number of organizations have issued a joint advisory recommending that any one who has a drug-eluting stent implanted should take blood thinners such as Plavix for a year after surgery.
 The advisory was issued by the American Heart Association, the American College of Cardiology, the Society for Cardiovascular Angiography and Interventions, the American College of Surgeons, and the American Dental Association.
The advisory was issued by the American Heart Association, the American College of Cardiology, the Society for Cardiovascular Angiography and Interventions, the American College of Surgeons, and the American Dental Association.The advisory referred to research which showed that up to 29 percent of patients who stopped taking their anti-clotting drugs too soon developed blood clots. Furthermore, of patients followed for 11 months after surgery, the group that stopped taking anti-clotting medication had a 7.5 percent death rate compared to a 0.7 percent death rate for those who continued taking their medication.
However, not everyone can take blood thinners for a year. People who require further surgery may suffer from bleeding problems if they are still on blood thinners. Additionally, the prohibitive cost of Plavix may be enough to prevent some people from taking it for a year. Plavix costs four dollars a day, which over the course of a year or longer can become very expensive.
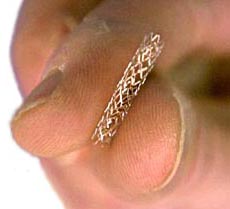
Drug-eluting stents have caused concern in the medical industry because of reports that the stents have a risk of blood clots which can block arteries. Compounding the problem is that, rather than occurring immediately following implantation, the clots may not occur until months or years after implantation.
Initially, medical professionals advised patients to use blood thinners for six to nine months following surgery in order to prevent blood clots. However, developments showing that the risk of blood clots still exists at least a year after surgery has led those professionals to now advise using blood thinners for at least a year. Blood clots can result in heart attacks or death.
Last week, the Wall Street Journal reported that Medicare is considering putting limits on coverage for drug-eluting stents. However, other officials have said that no such plan is in the works.
Drug-eluting stents are made by both Boston Scientific Corp., and Johnson & Johnson. The drug-eluting stent industry is estimated to be worth $6 billion a year. Drug-coated stents work by slowly releasing a medication that prevents arteries from reclogging after surgery.
In response to recent concerns regarding drug-eluting stents, the US Food and Drug Administration convened an advisory panel in December to discuss the risks of blood clots associated with the stents. The panel recommended that stents not be used for any off-label purposes (meaning the stents should not be used for anything not approved by the FDA). Approximately 60 percent of stents are implanted for non-approved uses.
The recommendation of a year for taking anti-clotting medication is just a guideline. Everyone responds to anti-clotting medication differently, so patients may be required to take Plavix for longer than a year. Furthermore, a patient's risk of bleeding and the situation surrounding the use of the stent may also have an impact on how long medication is necessary. Therefore, it is important to speak to a doctor regarding the length of time medication is needed.
If you have had a drug-eluting stent implanted and are taking blood thinners, do not stop taking your medication without first speaking to your doctor. If you have any surgeries scheduled make sure your doctor knows that you are taking a blood thinner. If at all possible, delay any elective surgery for at least a year after the stent is implanted.
